Tularemia
Other Names: Rabbit fever, hare plague, lemming fever, deerfly fever, Ohara's disease, yato-byo
Cause
Tularemia is a disease that can affect several organ systems. It is caused by the bacterium Francisella tularensis. Of the two most common subspecies, Type A is more virulent and associated with rabbits in a more upland cycle, while Type B is associated with aquatic rodents. Tularemia-like disease has been reported throughout history in humans in Europe, Japan, and the United states, but the bacterium was first isolated in the United States in 1911. Now F. tularensis is recognized as the cause of a multi-systemic, and at times fatal, disease of humans and animals.
Significance
Tularemia is a zoonotic disease meaning that it can be transmitted from infected animals to humans by certain vectors (listed below), inhalation, or ingestion of contaminated food or water. Humans are most often exposed when skinning or dressing infected rabbits. Human infections have been reported after running over rabbits with a lawnmower. Laboratory workers, veterinarians, landscapers, farmers, hunters, trappers, and cooks have increased risk of exposure to tularemia. Tularemia is listed as a possible bioterrorism agent because it is highly infective and has the potential to cause severe illness and death in humans.
Species Affected
F. tularensis has been reported in a broad range of host species including mammals, reptiles, birds, fish, and invertebrates. Rabbits and rodents are most commonly infected. Of the rabbits, hares and cottontail rabbits are important hosts. The most common rodent hosts include water voles, muskrats, lemmings, hamsters, and red-backed voles. The most commonly infected species in North America are cottontail rabbits, black-tailed jack rabbits, snow-shoe hares, beavers, and muskrats. Tularemia is occasionally reported in domestic cats and rarely in domestic dogs.
Exposure to infected rabbits accounts for 90% of human infections in the United States, and the majority of these are cottontail rabbits.
Distribution
Tularemia is present throughout North America, including the continental United States, Alaska, Canada, and Mexico. It has also been reported in central and western Europe, Africa, and several Asian countries including Russia and Japan. Tularemia is found primarily in the Northern hemisphere.
In 2004 an eastern cottontail rabbit in a Philadelphia, PA zoological park tested positive for tularemia, and in 2006 six more rabbits died of confirmed tularemia at the same park. An investigation following these deaths did not find F. tularensis in nearby ticks nor was the organism isolated from air samples. No human cases of Tularemia were reported. In 2011 a muskrat found dead in Crawford county, PA tested positive for Tularemia.
Transmission
Tularemia can be transmitted via the bite of blood-feeding arthropods including ticks, fleas, flies, and mosquitoes that carry the bacteria. The disease is also transmitted via inhalation of infected droplets or dust contaminated with infected tissues, feces, or urine. Consumption of undercooked infected animal tissue, and contaminated food or water can also result in disease. Waterborne outbreaks have been reported and are associated with aquatic rodents such as beavers and muskrats.
Clinical Signs
The disease lasts about 2-10 days in infected animals. Clinical signs are rarely observed in wildlife because they are usually found dead. Highly susceptible animals exhibit severe lethargy followed by death; infected animals are often slow, and may be captured easily. Less susceptible animals may have local inflammation or enlarged lymph nodes.
At necropsy animals that died of acute tularemia will have pale spots throughout the liver, bone marrow, and spleen. The lungs are often fluid filled and may have dark or firm areas. The liver and spleen may be enlarged. Less sensitive species are more likely to be chronically infected and will deteriorate in body condition.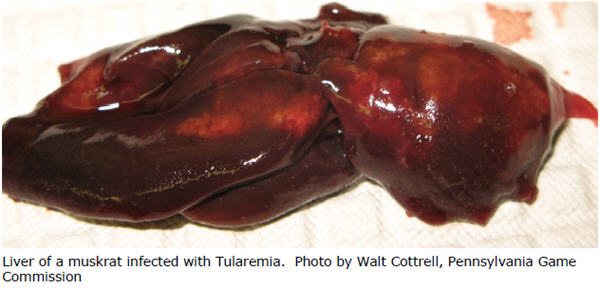
Diagnosis
Diagnosis is confirmed by isolating Francisella tularensis from the infected animal's blood or tissues.
Management/Prevention
Tularemia occurs naturally in wild rabbit and rodent populations. Increased rabbit and tick population densities can lead to an increase in the occurrence of the disease. Beaver and muskrat trappers are at a greater risk of waterborne exposure. Rabbit hunters and rodent trappers should be aware of the potential risk and should take precaution by wearing gloves, practicing simple hygiene, and cooking meat thoroughly (a meat thermometer should read at least 135° F). It is also important that trappers seek medical attention when a possible exposure occurs. People should also use insect repellent and promptly remove ticks to help prevent becoming infected.
Suggested Reading
Centers for Disease Control and Prevention (CDC). 2011. Tularemia. http://www.cdc.gov/tularemia/.
Foley, J. E., and N. C. Nieto. 2010. Tularemia. Veterinary Microbiology 140: 332-338.
Michigan Department of Natural Resources. Wildlife Disease. Tularemia. http://www.michigan.gov/dnr/0,1607,7-153-10370_12150_12220-27293--,00.html.
Morner, T., and E. Addison. 2001. Tularemia. Pages 303-312 in E. S. Williams and I. K. Barker, editors. Infectious diseases of wild mammals. Iowa State University Press, Ames, Iowa, USA.
Nigrovic, L. E., and S. L. Wingerter. 2008. Tularemia. Infectious Disease Clinics of North America 22: 489-504.
Sinclair, J. R., A. Newton, K. Hinshaw, G. Fraser, P. Ross, E. Chernak, C. Johnson, and N. Warren. 2008. Tularemia in a park, Philadelphia, Pennsylvania. Emerging Infectious Diseases 14: 1482-1483.
Tilley, L. P., and F. W. K. Smith, Jr. 2007. Blackwell's five-minute veterinary consult: canine and feline. Fourth edition. Blackwell publishing, Ames, Iowa, USA.